kk.Latest Update on Hunter: 6:40 PM CST — A Careful Warning About His Left Arm
Latest Update on Hunter: 6:40 PM CST — A Careful Warning About His Left Arm
At exactly 6:40 PM CST, doctors delivered an update that shifted the tone inside the room.
Measured. Clinical. But undeniably heavy.
They are now preparing for the possibility of skin grafting on Hunter’s left arm.
The final decision, however, will not come from imaging scans or surface exams.
It will come only when surgeons physically reopen the wound.
And until that moment, they simply don’t know.
Why Electrical Injuries Are So Unpredictable
Hunter’s trauma was caused by high-voltage electrical exposure — the kind of injury that behaves differently from standard burns.
In typical surface burns, tissue damage is often visible and measurable from the outside. But electrical injuries operate from the inside out.
The current travels along the path of least resistance — through muscle, fascia, nerves, and blood vessels — sometimes leaving skin deceptively intact while deeper structures quietly deteriorate.
Doctors describe it as a “hidden burn.”
On the surface, the skin may appear stable.
Beneath it, microvascular blood supply can collapse.
Muscle fibers can lose perfusion.
Fascia layers can begin to necrose without obvious external signs.
That’s why this next step matters so much.
The Only Way to Know: Surgical Exploration
No scan can fully confirm tissue viability in complex electrical trauma.
The only definitive assessment happens in real time — inside the operating room.
When surgeons reopen the wound, they will evaluate three primary indicators:
- Color of the tissue (healthy muscle appears red and well-oxygenated)
- Bleeding response when gently incised
- Perfusion quality, or how well blood is actually reaching the tissue
If the muscle contracts and bleeds appropriately, it’s a promising sign.
If it appears pale, gray, or nonreactive, that suggests deeper compromise.
In these moments, millimeters matter.
And right now, the answers are sealed beneath sutures.
What Skin Grafting Would Mean
The word “grafting” can sound alarming. But in severe trauma care, it is often protective rather than cosmetic.
If surgeons determine that underlying tissue failed to fully recover, they may need to transplant healthy skin — typically harvested from another part of the body — to:
- Cover exposed structures
- Reduce infection risk
- Restore barrier function
- Stabilize long-term healing
This step would not represent failure.
It would represent reconstruction.
Skin grafting in electrical injuries is about creating a stable environment for deeper tissues to recover — especially when the body cannot regenerate sufficient coverage on its own.
But the need for grafting would confirm that certain areas did not regain adequate blood flow.
And that possibility is what makes the next 24–48 hours so pivotal.
The Mood Shift at 6:40 PM
Until this evening, monitoring focused primarily on pain control, infection prevention, and circulation stability.
Today’s update introduced a new layer of uncertainty.
Doctors explained that while surface healing has appeared steady, subtle indicators suggest deeper tissue may not be perfusing as strongly as hoped.
It’s not definitive.
But it’s enough to warrant surgical reassessment.
When physicians say, “We don’t know yet,” it isn’t hesitation.
It’s honesty.
Electrical injuries evolve. Tissue that appears viable one week can declare itself nonviable the next as blood supply falters or inflammation escalates.
That delayed declaration is what makes these injuries so complex.
Hunter’s Condition Tonight
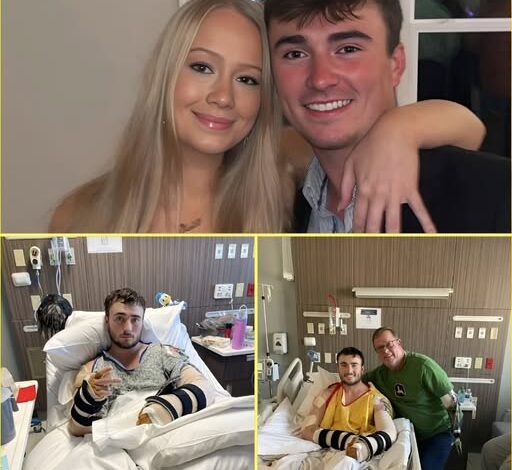
Hunter remains in pain but alert.
He is conserving strength ahead of the next evaluation window. Vital signs remain stable. Infection markers are being closely tracked. Circulation to the extremity is present, though described as fragile.
Pain management continues around the clock.
There has been no dramatic crash.
No sudden emergency.
But there is weight in the waiting.
Because the next reopening will determine whether his body is rebuilding from the inside — or whether reconstruction must go further than hoped.
The Tissue Marker Surgeons Are Watching
Before reopening the wound, doctors are closely monitoring one specific factor: tissue perfusion stability over time.
Electrical injuries create what trauma specialists call a “zone of stasis” — tissue that exists in a gray area between survival and necrosis.
In this zone, survival depends entirely on whether microvascular blood flow can sustain recovery.
If perfusion improves, the tissue strengthens.
If it declines, grafting becomes necessary.
That dynamic process is why timing matters.
Open too early, and tissue that might recover could be removed unnecessarily.
Wait too long, and infection risk increases.
The balance is delicate.
Why the Next 48 Hours Matter
In high-voltage trauma, the body doesn’t reveal its final condition immediately.
Inflammation peaks. Swelling shifts. Microcirculation recalibrates.
The coming 24–48 hours will determine:
- Whether deeper muscle layers maintain viable blood supply
- Whether protective coverage can heal naturally
- Or whether surgical grafting becomes the safest path forward
If perfusion is stronger than expected, it could accelerate recovery dramatically.
If not, reconstruction may extend the timeline — but still offer a stable, protective outcome.
Either way, action will be based on precision — not assumption.
A Fight Still Being Fought
Hunter’s journey has already defied initial fears. Surviving high-voltage electrical trauma is itself extraordinary.
Now, the focus shifts from survival to structural integrity.
From stabilization to rebuilding.
He remains mentally present. Determined. Quietly bracing for what comes next.
Tonight, there are no final answers.
Only preparation.
Only monitoring.
Only the understanding that beneath those sutures lies the truth of how deeply his body is healing.
And soon, surgeons will look directly at it.